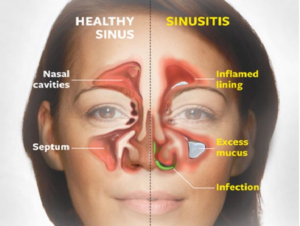
One of the leading causes of disease and mortality in people is respiratory tract infections (RTI). Viruses are a common cause of RTIs, which frequently make immune systems sicker for longer periods of time. To research interactions between respiratory viruses and the host and to test new treatment interventions, it is necessary to develop reproducible and scalable in vitro culture models that precisely replicate the human respiratory system.
To investigate how various types of airway cells and respiratory viruses interact, numerous in vitro respiratory systems for cell culture including human nasal epithelial cells and alveolar epithelial have been designed. Most of these models are still based on immortalised cell lines. Such unicellular systems fail miserably in providing comprehension of the events that take place at an integrated tissue level, even though they are beneficial in the research of acute viral infection and reproduction mechanisms at a molecular and cellular level.
To fully understand infection kinetics in connection to innate immune response, microbiota, immune cells, and other aspects including inherent cellular mechanisms of resistance, we need far more sophisticated models. For some time, new in vitro models have been suggested and used, particularly lung epithelial cells. Airway organoids, created from mesenchymal stem cells, are a type of 3D culture that has just been established and shows promise as an effective method for studying host-pathogen interactions.
Applications of Primary Epithelial Cells in Infection Studies
Human epithelial cells can resemble host lifestyle variables like a history of smoking and obesity. Epithelial cells are helpful for researching virus stability in various environmental settings. For instance, the effect of humidity levels on the durability of a pandemic influenza A virus in aerosols and droplets was investigated using bronchial epithelial cells.
In vitro studies of respiratory virus pathogenesis using primary cell models may provide a reliable representation of viral infection in the host. They can be used to study innate immune responses in respiratory epithelial cells, discover viral receptors, determine viral tropism, imitate sickness, and more.
Continuous cell lines exert selection pressure on viruses, causing them to adapt to culture even despite their ability to provide fundamental insights into the relationships between viruses and their hosts. The capability of genetic alteration, which is currently not attainable in primary respiratory cell cultures, is among the benefits of continuous cell lines. The use of organoids produced from human stem cells, which could be designed to express desired host traits, could help to overcome this obstacle in the future.
Conclusions
In vitro models that accurately mimic the intricacy of our RT and the series of processes that take place during viral infections must be scalable, practical, inexpensive, and reproducible.
Primary HAEC is more appropriate than cell lines for studying fundamental viral-host interactions, such as the utilisation of receptors and the tropism of a respiratory virus. However, AO seems more appropriate for examining the intricate interactions between viruses, target cells, and immune responses.
To even better replicate the microenvironment present in the RT, this model needs to be improved by including additional system components, such as endothelium, airflow, commensal bacteria, and immune cells. This culture method will aid in our understanding of viral respiratory infections, host responses, and the development of potent antiviral treatments.